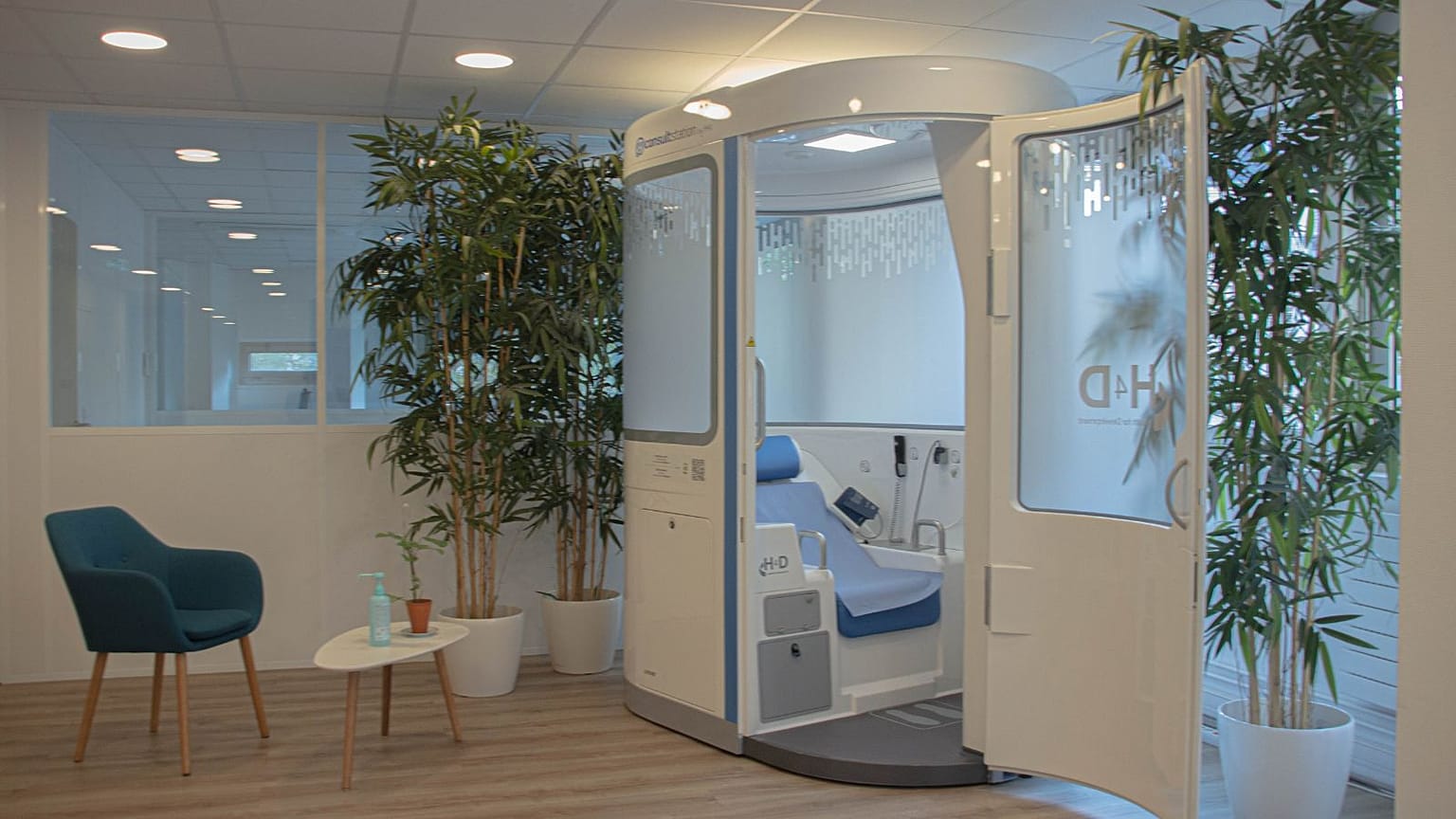
Inside this hi-tech telemedicine cabin, patients carry out their own physical exam, guided by a doctor on a video call. I gave it a try.
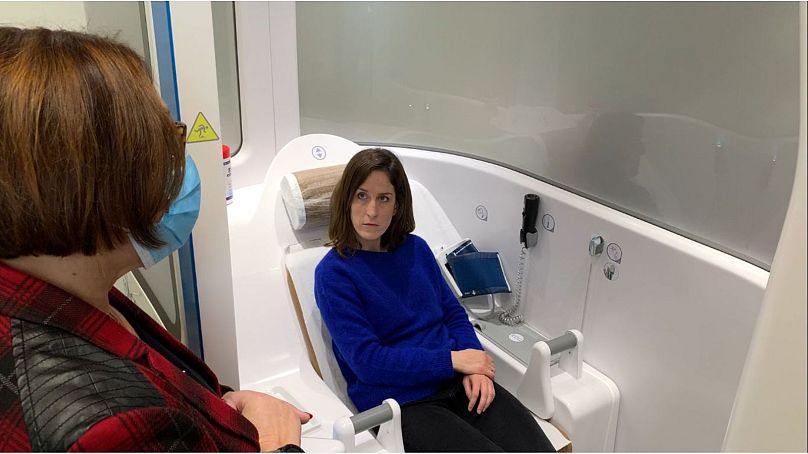
A friendly face appears on the screen and so begins what could be yet another Zoom call – except I’m sitting inside a white booth that looks like a doctor’s office designed to fit on an airplane, and I’m a little nervous.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
Attached to the walls are a stethoscope, a blood pressure monitor, an oximeter and other scopes that I will be instructed to use on myself throughout my teleconsultation.
As France struggles with a shortage of doctors, its worst-hit regions are rolling out hi-tech telemedicine booths, where patients can conduct their own checkups while on a video call with a physician in another part of the country.
It’s a slightly surreal experience, as I found out firsthand, and a controversial solution to a very human problem being repeated across Europe.
While France’s healthcare system is often hailed as one of the best in the world, it’s facing a demographic crisis in which doctors are getting older and are not being replaced where they’re needed the most.
According to government data, nearly 7 million people in France – one in 10 – don’t have a referring general practitioner (GP), and 30 per cent live in a medical desert.
Those are regions where it’s nearly impossible to see a doctor because there simply aren’t any nearby, or because the few in the area are so busy they don’t take new patients.
In places like Montréal-la-Cluse, a village east of Lyon close to the Swiss border, authorities are now hoping tech can help fill the gap.
“This is a very dynamic region economically, and we regularly have more people settling here. So the population is growing, the needs are growing, but our doctors are getting older, and when they retire, they’re unfortunately not being replaced,” said Murielle Derderian, manager of a local pharmacy.
Just next door, in the town’s health centre, sits the “Consult Station” – a hi-tech booth made by start-up H4D, whose connected medical instruments allow patients to conduct their own physical exam while speaking to a doctor on a screen.
Playing doctor
Inside, you follow the physician’s guidance and manipulate the tools yourself to take your temperature, blood pressure, blood oxygen level and heart rate.
Other scopes allow you to check the inside of your ears and mouth and share the high-definition imagery with the doctor in real time.
The doctor instructs you to insert these at the right angle and to adjust the focusing wheel a bit like you would using binoculars – except here, your target is not a rare bird but your swollen tonsils or your infected eardrum – until a shockingly sharp image appears on the screen.
It’s graphic – way more information than you would get from a normal consultation, as you’re now seeing what the doctor sees, and it won’t look pretty if you’re sick.
Dr Arnaud Mehats, the general practitioner who guided me through my trial consultation, said the H4D booth was especially useful when it comes to ears, nose and throat (ENT) pathologies like rhinopharyngitis, a sore throat or a sinus infection, as well as pulmonary pathologies like asthma and bronchitis.
“For all of this, it's like being in a doctor's practice. There’s no difference in terms of the quality of the physical examination,” he said.
Using a connected dermatoscope, patients can also flash a light on specific moles and freckles. They will appear on the screen as if under a microscope and help the doctor assess remotely whether any of them look suspicious and need further checks.
Handling all these applications requires a powerful Internet connection, so H4D partnered with Bouygues Telecom to provide a wireless 5G hotspot together with the booth.
“We could even connect it to a satellite if needed,” the company’s managing director Valérie Cossutta told Euronews Next.
Local authorities paid €100,000 to install the booth in October 2020, at the height of the COVID-19 pandemic. It now sees about 30 patients a week, and several others have been deployed across the region.
No other choice
Of course, there are limitations to the tech. Patients are screened for this booth when they make their appointment online. For instance, they cannot make a booking if they have gastrointestinal, neurological or haemorrhagic symptoms.
And if anything alarming occurs during the teleconsultation, the doctor can directly alert emergency services, which will come to pick the patient up directly at the booth.
While the tech may seem intimidating, there are also staff inside the medical centre to guide patients, give instructions and disinfect the booth after each consultation.
“What’s important is that the patients who come here get a medical answer and know that they can come back, which they often do. Some patients come back because unfortunately, in the meantime, they have not found a doctor,” said Caroline Millet, who looks after the booth in Montréal-la-Cluse.
A teleconsultation costs €25 to €30, the same as a normal visit to the doctor.
But not everyone in the village is willing to give it a go. Several elderly people quizzed in the neighbouring pharmacy said they were put off by the very idea of not seeing a doctor in person.
Others who tried the cabin said it was certainly better than nothing.
“Overall, the patients who’ve used this booth are very satisfied,” said Derderian, the pharmacy manager. “But I see it only as a temporary fix. It's not a sustainable solution, and it doesn’t fit with the idea we have of a family doctor, and the ability to follow up”.
‘Why can’t doctors also work from home?’
H4D has rolled out around 140 of its booths so far and it has another 100 in the works, mainly smaller and cheaper ones designed for offices. Its main market is France, but these days it’s also shipping to Italy, Portugal, and the UK.
Other companies such as Medadom and Tessan are rolling out hundreds of telemedicine booths across health facilities, pharmacies, and even grocery stores across France.
“It’s important that everyone has access to healthcare,” Cossutta said. “But the way doctors and the population are spread out is uneven, so with telemedicine cabins, you solve part of that equation”.
Companies argue that the COVID-19 pandemic has made telemedicine much more acceptable to patients, and the tech around it is getting smarter and smarter.
Another start-up, i-Virtual, has just received EU certification for its new contactless diagnosis technology, which can monitor vital signs using just a 30-second selfie video. ‘Caducy’ measures a patient’s heart rate, respiratory rate and stress level by analysing how the blood flows through their skin.
The company says a clinical trial on over 1,000 patients showed 95 per cent accuracy. It now hopes to license the tech to teleconsultation and telesurveillance platforms, to provide healthcare professionals with quick insight into their patients’ vital signs.
There’s no need for patients to manipulate any complicated instruments, nor to disinfect them after each consultation, said Myriam Benfatto, marketing manager at i-Virtual.
“It reduces unnecessary trips to a doctor’s office and can easily be added to a tablet that a nurse could carry around from one patient to the next, instead of taking their vitals each time – it’s much quicker,” she explained.
Asked what doctors made of the technology, she said there were “two schools”.
“One school is more traditional and reluctant about digital health. But others are very enthused at the prospect of saving time. They realise that digital is part of our lives,” she said.
“One doctor recently told me: ‘why can everyone work from home, but not doctors?’ His point was that they too should be able to do some things remotely”.
For more on this story, watch the video in the media player above.