With over a million people already infected and 50,000 fatalities, the race is on to find a cure for COVID-19, the virus which has arguably caused the most serious global crisis since World War II.
SARS-Corona virus 2 (SARS-CoV2), cause of COVID-19, is the infection that the whole world is now trying to beat. The respiratory disease has arguably caused the most serious global crisis since World War II, infecting over one million people and causing more than 70,000 deaths.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
As the world grapples with the pandemic, the scientific community is on the hunt for effective, scalable treatments, while at the same time developing a safe and tested vaccine.
The race to find a vaccine
It usually takes 10 to 15 years to develop a vaccine.
"For Ebola, we did it in five years, I know we can accelerate that," says Seth Berkley, the CEO of the global health partnership GAVI (Global Alliance For Vaccines and Immunization).
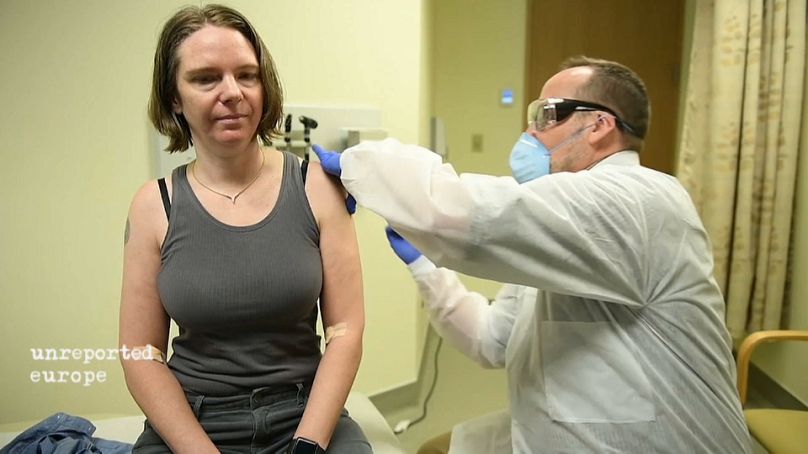
Highly unusually, human trials with an experimental COVID-19 vaccine have already begun. Seattle resident Jennifer Haller became the first person to receive one on March 16 2020, at her hometown's Kaiser Permanente Washington Research Institute.
She was one of a group of volunteers that were involved in testing on humans just weeks into the fast-spreading epidemic.
This experimental vaccine, officially named mRNA-1273, was developed by the National Institutes of Health and Massachusetts-based biotechnology company Moderna Inc. There’s no risk of the volunteers becoming infected, because the shots do not contain the coronavirus itself.
The World Health Organization says there are over 40 potential vaccines. There are reportedly as many as one hundred undergoing development, although only a handful are as yet being clinically tested.
The promise of RNA vaccines
A promising way of combating COVID-19 appears to be with a vaccine that manipulates a part of the virus known as RNA.
"The RNA molecule carries all the coronavirus' genetic information," explains Marie-Paule Kieny, Director of Research at the French Public Health organisation INSERM. "The RNA can be synthesised on a large scale in the laboratory. This is why it's being used in this first vaccine, for which there are clinical trials underway.
"Other vaccines are based on viral DNA, or on other viruses which have been weakened, which don't produce disease and in which we can include the genetic information of the COVID virus."
There are over thirty companies and academic institutions worldwide trying different approaches to find the silver bullet that will beat COVID-19.
The Trump-Curevac controversy
In Germany, the biopharmaceutical company Curevac is using the so-called messenger molecule - mRNA - in a vaccine that it believes will be ready for clinical tests in June.
As Curevac spokesperson Thorsten Schüller explains:
“We use the mRNA to instruct the body to produce its own vaccine, so we only put information into the body. It's a totally new approach in medicine.”
Curevac made the front pages when it was reported that US President Donald Trump had offered the company one billion dollars to secure the vaccine exclusively for the United States. But Schüller insists the company never received any such offer from the White House or any other US institution:
"Our aim is to develop a vaccine for all people, all over the world. Then the health practitioners have to decide how to distribute such a vaccine.”
Ursula von der Leyen, President of the European Commission, has since offered CureVac 80 million euros in research funding to help develop a vaccine.
Controversial treatments
While the world waits for a vaccine, potentially millions of patients will need treatment. Researchers and doctors have started to test sometimes controversial combinations of existing drugs to treat those infected, but so far there is no cure.
In France, Marseille's University Hospital Institute has offered to test and treat people exhibiting COVID-19-like symptoms. Didier Raoult, head of the institute's infectious diseases department believes that a cheap and easily produced malaria drug can treat COVID-19. Raoult announced promising results on a small sample of patients in late February using Chloroquine and its related compound Hydroxy Chloroquine.
But Marie-Paule Kieny is one of many in the scientific community that are sceptical:
"I know that there's been a lot of talk, in France and elsewhere, about claims by certain researchers who say that this drug works, that this drug will save the world. But unfortunately, for the moment, the proof that this hydroxychloroquine medication is effective is extremely weak, or even non-existent.”
Across the border in Italy, doctors at Milan’s San Raffaele Hospital are using the same combination of drugs suggested by Professor Raoult.
Fabio Ciceri, San Raffaele's Deputy Director explains there are no nationally-approved protocols and each hospital can choose its strategy:
"AIFA, the Italian Medicines Agency, has instructed us on a reasoned use of the drugs. So the drugs we are using are existing drugs, repurposed to be used against the coronavirus, based on laboratory results that demonstrate their potential to be effective".
Unheeded warnings
It's felt by some that the current pandemic could have been avoided, or at least very much better prepared for.
After all, there have been previous coronavirus outbreaks, beginning with SARS in 2003.
In 2015, the software developer and philanthropist Bill Gates gave a Ted Talk in which, three years after the MERS outbreak, he warned that the world was not ready for a future pandemic**.**
“If anything kills over 10 million people in the next few decades it’s most likely to be a highly infectious virus, rather than a war. Not missiles, but microbes.
"Part of the reason for this is that while we have invested a huge amount in nuclear deterrents, we have actually invested very little in the system to stop an epidemic. We are not ready for the next epidemic.”
The warnings of Gates and others went largely unheeded. Some prominent epidemiologists blame a system more focused on commercial opportunities than public health needs.
Stuart Blume, Professor of Science and Technology at the University of Amsterdam agrees that despite the attention the issue has received globally, practical organisation and preparation was definitely lacking:
"All the countries for the last 10 years have been busy with epidemic preparedness scenarios. But they're still all over the place (in terms of) trying to find what to do.”
Ildefonso Hernández Aguado, Professor of Preventive Medicine and Public Health, at Alicante's Miguel Hernández University says the worldwide financial crisis which began in 2008 influenced this lack of preparedness:
“Previously, drills were carried out with a certain frequency to get ready for these events. This came to a halt because of the post-crisis years of austerity.
"Budget cuts were requested and money was saved in sectors that were thought to be inessential. What’s happening could have been foreseen, but policies and decision-making went the other way”.