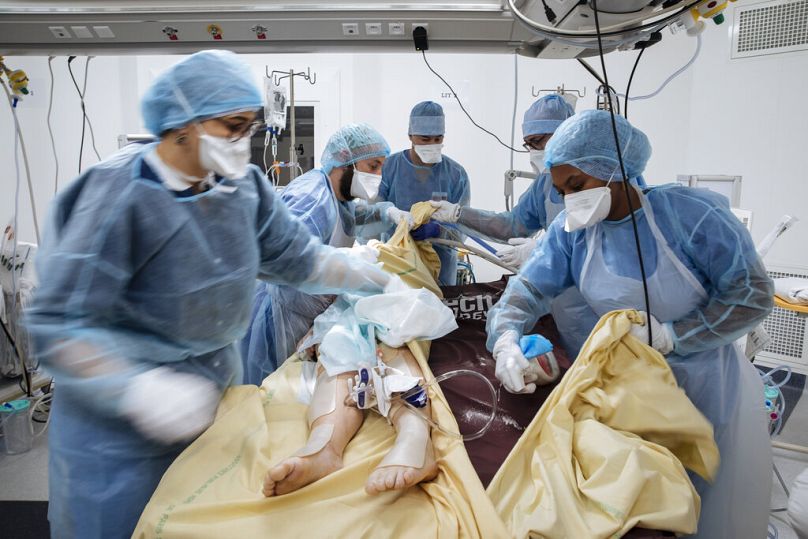
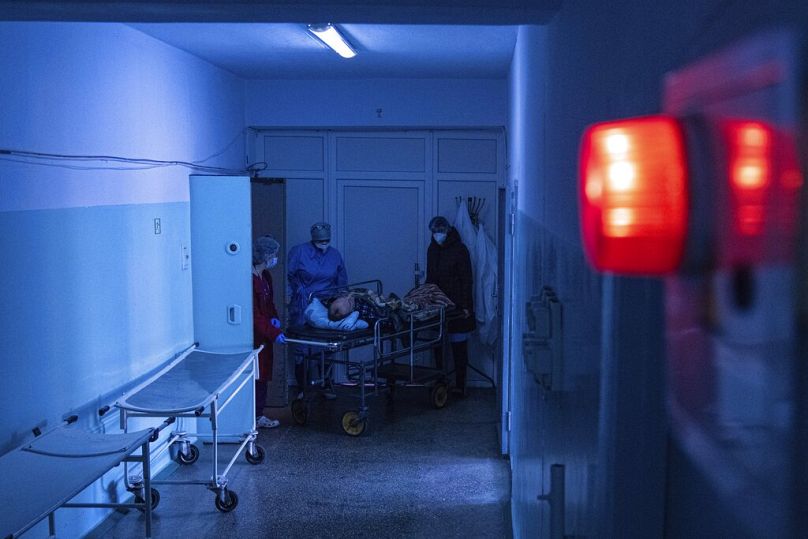
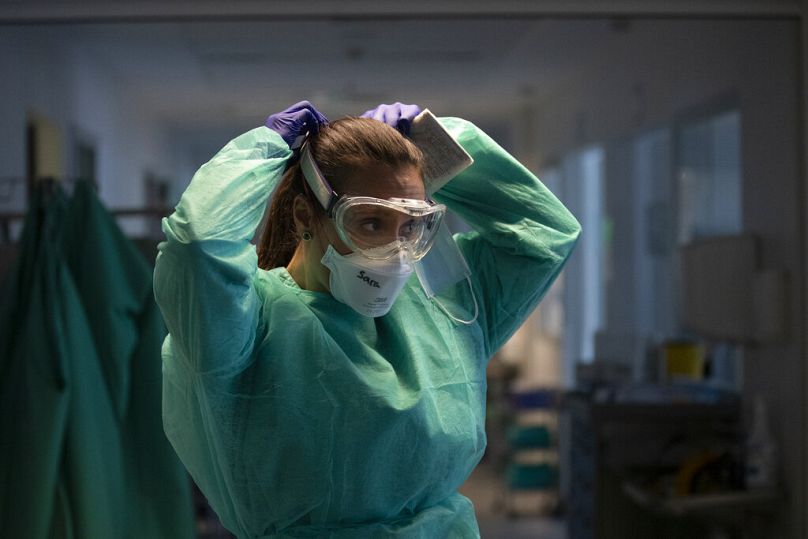
At least 80 per cent of critically ill COVID-19 patients are unvaccinated, putting them and others at risk. Europe's intensive care staff need help to tackle this crisis, write the president and president-elect of the European Society of Intensive Care Medicine
In late August, the European Commission announced an essential milestone in the evolution of the COVID-19 crisis.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
Reaching the EU’s 70 per cent target for the full vaccination of adults was an important step in our shared progress towards a safer future for all Europeans.
But with winter approaching, we can already see that more effort needs to be made to increase the numbers. ICUs are facing a new surge, comprising mainly the unvaccinated minority.
Both the unvaccinated, and those at risk who received their first two doses more than six months ago, should urgently receive new COVID-19 jabs.
ICU admission data reveals the consequences of low vaccine uptake
In Europe, tens of millions of eligible adults are still not vaccinated. The sad and avoidable reality is that this increases the risk of those who reject the vaccine ending up in an ICU if they contract COVID-19, unnecessarily limiting some of society’s most valuable finite resources: ICU beds and medical staff.
This translates into adverse outcomes for both COVID-19 patients for whom ICU beds might be lacking, but also for non-COVID-19 patients whose medical and surgical care could be delayed or even cancelled.
The severe consequences of low vaccine uptake are reflected in intensive care admission statistics published by many EU member states: at least 80 per cent of critically ill COVID-19 patients are now the unvaccinated.
The average stay of a COVID-19 patient in an ICU lasts about three weeks, meaning a single COVID-19 patient needs an ICU bed and staff for three times longer than the average non-COVID-19 patient.
Many types of surgery require a patient to spend only a few days recovering in an ICU afterwards. The unavailability of beds for such short but mandatory stays has forced operations to be postponed in times of COVID-19 surges.
Impact of severe COVID-19 doesn't end on discharge
For the unvaccinated who are fortunate enough to survive COVID-19 in an ICU, the experience often serves as a stark wake-up call.
The ordeal of ICU COVID-19 treatment is as brutal physically as it is mentally, and it does not end on discharge.
Weeks of sedation and ventilation can leave patients emaciated, making normal daily tasks physically challenging, complicated further by 'brain fog' and the mental trauma of a near-death experience.
Post-intensive care syndrome can affect both patients and their families, with post-traumatic stress disorder, in particular, having dramatic medical and socioeconomic consequences.
Properly staffed ICU beds are necessary to maximise the quality of care and chances of survival. They are also necessary to avoid or reduce the development of post-intensive care syndrome.
This is only possible if the rate of severe infections is kept under control with vaccinations and public health measures.
Help ICU staff by combatting the 'infodemic'
Knowing that a vaccine is available to help prevent critical illness in these patients is a deeply saddening change in the day-to-day work of ICU staff.
Nonetheless, medical professionals in intensive care medicine remain committed to helping every single patient requiring care.
They have shown this by repeatedly going above and beyond to save lives during the pandemic. All the while, 20 per cent of ICU capacity is closed due to shortages in nursing staff: a persistent problem that needs to be urgently addressed.
We need the support of citizens, the media, and policymakers. Misinformation needs to be combated at every opportunity, with the right support given to individuals to make the right choice.
We are committed to developing initiatives to fight the 'infodemic' and provide clear, truthful and honest information to every single person so as to better inform their choices.
Build up an EU reserve of ICU doctors and nurses - now and for challenges to come
Policymakers, meanwhile, must turn their attention to the evolution of Europe’s ICUs.
It is a positive development that there have been increases in ICU capacity in some countries. But it would be a mistake to think we can decrease COVID-19 because we have more beds.
Reinforcing the strength of the last line of defence is important, but is no replacement for broader public health measures.
COVID-19 has taught us that in a globalised society, a pandemic cannot only be fought locally: a lesson that applies just as much to our ICUs.
On behalf of Europe’s intensive medicine staff, ESICM calls on EU policymakers to develop a long-term European strategy for ICUs.
We must establish a reserve of doctors and nurses with intensive care competencies, and ensure the rights of intensive care professionals to transfer their skills beyond their borders to other ICUs in response to public health crises.
Breaking down these barriers would not only serve Europe for the duration of this pandemic but also in every future crisis with the potential to threaten the functioning of our healthcare systems.
Prof. Maurizio Cecconi is president of the European Society of Intensive Care Medicine (ESICM) and chair of the Department of Anesthesia and Intensive Care Units at Humanitas Research Hospital in Milan. Prof. Elie Azoulay is president-elect of ESICM and head of the critical care department of Saint-Louis Hospital in Paris.