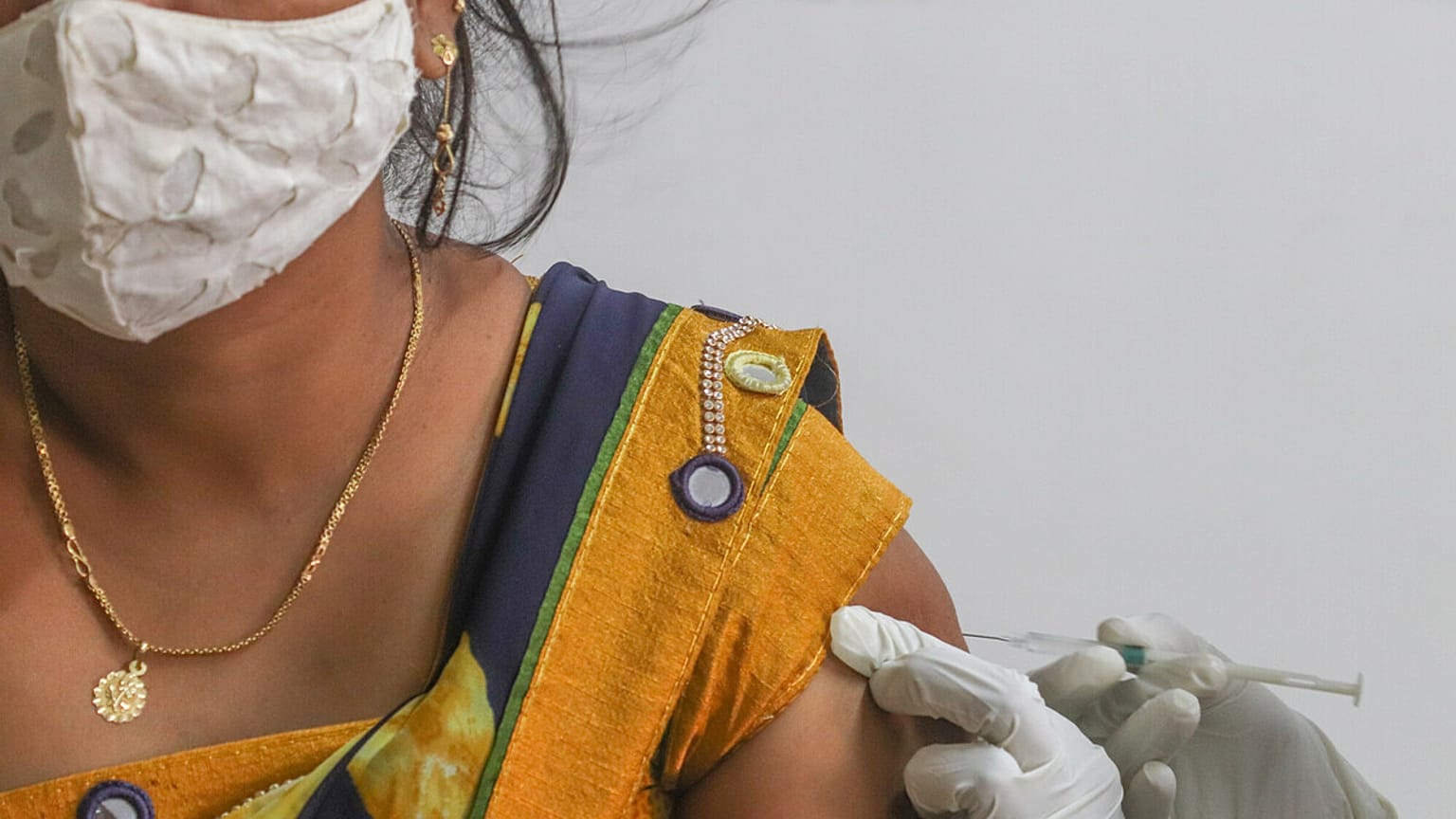
To end the global Covid pandemic, richer nations need to focus their vaccines, health technologies and finance on poorer countries too.
The views and opinions expressed in this article are those of the author.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
The Omicron variant is swiftly taking over the global news agenda. One theory under discussion is that Omicron may have evolved in a COVID-19 patient living with untreated HIV, due to their suppressed immune system failing to control repeated mutations of the virus.
While we may never know, this theory is gaining traction, both in the scientific and global development communities. If it is true, the emergence of Omicron is a stark warning, that if we continue to leave parts of the world behind on access to treatment and vaccines, we will never be rid of COVID-19.
AIDS remains a pandemic
Across the globe, there are nearly 38 million people currently living with HIV, two-thirds of whom (67 per cent) live in Sub-Saharan Africa. There are long-running inequalities between regions in HIV prevention, treatment, and diagnosis, and worryingly, these have been hugely exacerbated by Covid-19.
2020 saw huge disruptions to HIV services across the globe. HIV prevention and treatment services, schooling and violence-prevention programmes have all been impacted, with health systems and communities pushed to the brink.
These colossal challenges have been so detrimental, that UNAIDS warns they may send the progress made against AIDS over the past 40 years into reverse.
In a report released this week, UNAIDS warned that if leaders fail to tackle the inequalities holding back progress on HIV, the world could face 7.7 million AIDS-related deaths over the next 10 years.
These figures are a tough wakeup call, both that the global community is failing people living with and at risk of HIV, and that COVID-19 has increased the urgency with which existing pandemics must be tackled.
Omicron is a stark new warning
The issue of COVID-19 potentially lingering longer among people living with HIV but unable to access treatment is hugely concerning.
Not only does it risk the health and even lives of people with HIV in low-income countries - it also acts as a warning that faltering progress towards ending existing pandemics such as HIV ultimately makes the world a less safe place.
Yet currently, the global community has its sights elsewhere. For the past few months, pandemic preparedness and response (PPR) has been at the top of every agenda.
We’ve seen new bodies dedicated to PPR springing up, including the Independent Panel for Pandemic Preparedness and Response, the Pandemic Preparedness Partnership, and the G20's High-Level Independent Panel to name a few.
This week, the World Health Assembly is meeting to agree on a new mechanism for pandemic preparedness worldwide.
Yet there is a wider trend here, one which sees the governments of rich countries moving on from a problem as soon as it appears to be in someone else’s back yard.
We have seen this with AIDS, where the transformative impact of HIV treatments in high-income countries has seen urgency, focus, and funding for the global response fall sharply, and we are starting to see it with COVID-19 too.
This latest pandemic is far from over, but there is a clear risk that high-income, high-vaccination countries are already pivoting sharply towards viruses that don’t exist yet while turning a blind eye to those that continue to impact the Global South.
Equity is the way out of all pandemics
This much we know - pandemic responses fail when vaccines, health technologies and financial support are available to some and not to others.
The COVID-19 vaccine apartheid has been a prime example of this. For the past year, we’ve seen wealthy nations hoard vaccines, while low- and middle-income countries have been left exposed to the full force of successive waves of COVID-19 infections and dangerous new variants.
At the beginning of November 2021, just 2 per cent of people in low-income countries were fully vaccinated against COVID-19, compared to 65 per cent in high-income countries.
These shocking inequalities echo the treatment inequalities of the early response to AIDS and we cannot allow them to continue. For as long as Covid-19 is left to rage unchecked in large parts of the world, we will never be free of it. The same can be said for AIDS, TB, and every other infectious killer.
Pandemic preparedness and existing pandemics
The only way out of this pandemic, and to prepare for future health threats, is to invest in the responses to those which the world is already dealing with, and address the issues of inequality that are holding them back.
We know that many of the capabilities required to detect, prevent and respond to future health threats – from surveillance and supply chains to drug manufacturing and rollout – mirror exactly those needed to fight existing health threats like AIDS or Malaria.
So instead of diverting funding away from existing health issues, countries should instead increase financial resources for global health and develop strategies that not only protect against future pandemics, but also give communities the skills, tools, and money they need to tackle existing ones, such as HIV and COVID-19.
It would be counterproductive to consider the issues of pandemic preparedness, strengthening health systems, including community structures of those systems, and ending existing pandemics in silos – these must be considered as one.
It should not take the emergence of a new COVID-19 variant to highlight the importance of tackling all pandemics with equal regard.
The global community must have a shared goal – of ending existing pandemics, whilst also increasing the overall resilience of health systems and increasing the capacity of nations across the globe to anticipate future health threats.
Ultimately, only this cohesive action has the power to keep our populations safe – well into the future.
- Christine Stegling is the Executive Director of Frontline AIDS