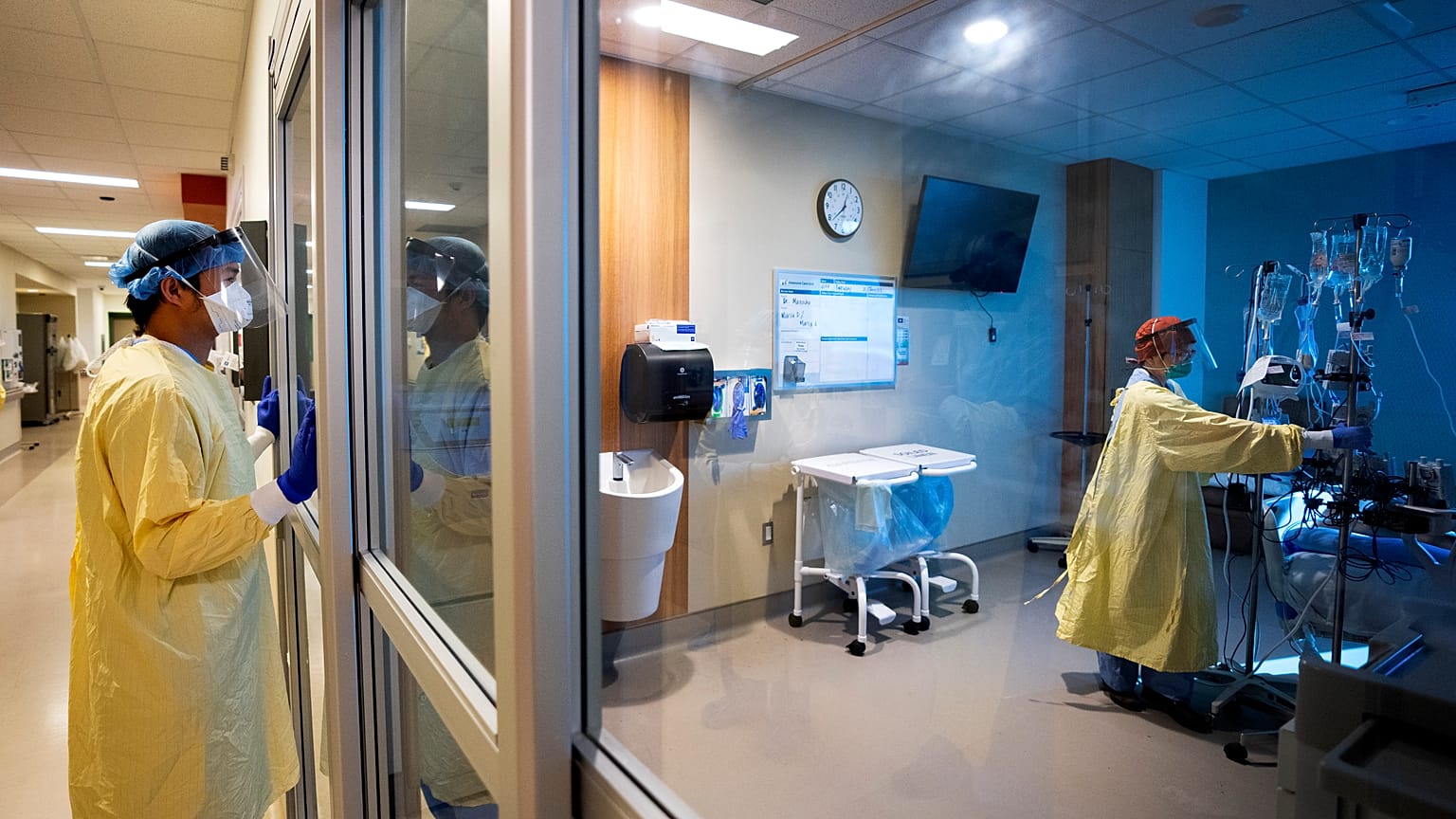
Cognitive impairment, such as difficulty recalling words, could also be affecting many people who have had COVID-19 but were not hospitalised, the study found.
A severe case of COVID-19 infection could cause cognitive damage equivalent to 20 years of ageing, according to a new study.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
The impact on the brain is similar to that experienced between the ages of 50 to 70, scientists said, adding that it is the equivalent of losing 10 IQ points.
There is a growing body of evidence showing that coronavirus infection can have consequences beyond the initial illness, with many people seeking medical advice over “long COVID” symptoms.
Reported long COVID symptoms include fatigue, “brain fog”, problems recalling words, sleep disturbances, anxiety and more, months after infection.
Between a third and three quarters of hospitalised patients report to still be suffering cognitive symptoms three to six months after acute illness, and this can occur even in mild cases.
Loss of 10 IQ points
The findings from the team of scientists at the University of Cambridge and Imperial College London in the UK suggest the effects of infection are still detectable more than six months after the acute illness.
The researchers analysed data from 46 people who were hospitalised with COVID-19 on the ward or intensive care unit at Addenbrooke’s Hospital in Cambridge, between March and July 2020.
Sixteen of these patients were put on mechanical ventilation during their stay in hospital.
They were put through computerised cognitive tests an average of six months after their acute illness, measuring aspects such as memory, attention, and reasoning.
Comparing their results against a control group, the team found the patients were less accurate and slower at responding, with effects strongest for those who were on mechanical ventilation.
They estimate the cognitive loss is similar to that experienced between the ages of 50 to 70, or the loss of 10 IQ points.
Professor David Menon from the Division of Anaesthesia at the University of Cambridge, the study’s senior author, said: “Cognitive impairment is common to a wide range of neurological disorders, including dementia, and even routine ageing, but the patterns we saw – the cognitive 'fingerprint' of COVID-19 – was distinct from all of these.”
“We followed some patients up as late as 10 months after their acute infection, so were able to see a very slow improvement,” he added.
“While this was not statistically significant, it is at least heading in the right direction, but it is very possible that some of these individuals will never fully recover.”
Difficulty finding words
One of the tasks patients scored particularly poorly on was verbal reasoning, a finding that supports a commonly-reported issue post-COVID: difficulty finding words.
They also found slower processing speeds, aligning with previous observations post COVID-19 of decreased brain glucose consumption within the frontoparietal network of the brain, responsible for attention, complex problem-solving and working memory, among other functions.
The researchers say several factors could cause the cognitive deficits, such as inadequate oxygen or blood supply to the brain, blockage of blood vessels, microscopic bleeds, or, as backed up by emerging evidence, damage caused by the body’s own inflammatory response.
They added that even people not sick enough to be admitted to hospital may have these signs of mild impairment.
Professor Adam Hampshire from the Department of Brain Sciences at Imperial College London, the study’s first author, said: “Around 40,000 people have been through intensive care with COVID-19 in England alone and many more will have been very sick, but not admitted to hospital. This means there is a large number of people out there still experiencing problems with cognition many months later. We urgently need to look at what can be done to help these people.”
The findings were published in the journal eClinicalMedicine.