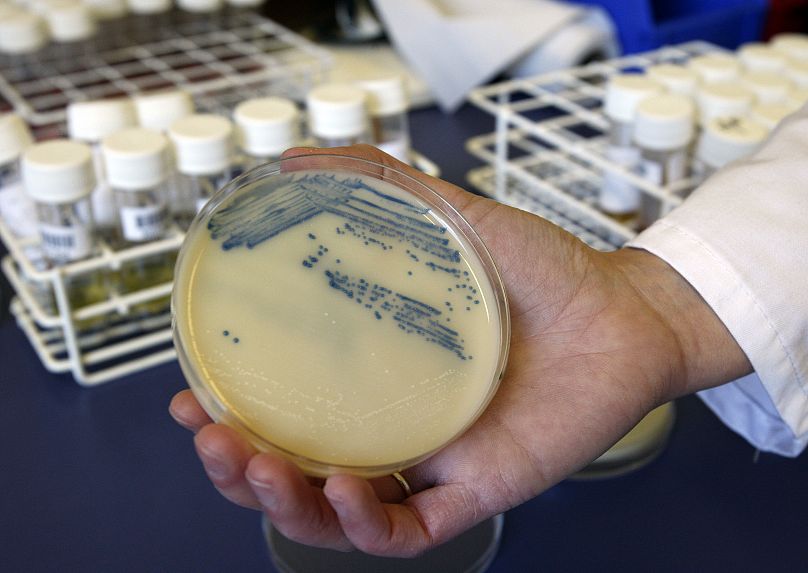
A new four-part series in the Lancet details how so-called superbugs are impacting global health and how preventing bacterial infections in the first place could reduce drug resistance.
Ramping up basic infection control measures could prevent 750,000 deaths linked to antibiotic resistance per year in developing countries, according to a new study.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
Antimicrobial resistance, when bacteria, viruses, or other microbes no longer respond to medicine, is a global public health threat, with researchers estimating that nearly 5 million deaths globally are associated with it.
It is mainly driven by the misuse and overuse of antibiotics in humans, animals, and plants, experts say.
In a new four-part series published on Thursday in the Lancet, researchers recommend new global targets to tackle bacterial pathogens and their resistance to medicine.
They also quantified how promoting vaccination, providing access to safe water, and preventing hospital infections could stop these bacterial diseases before drugs are needed.
“In many low and middle-income countries, there are perfectly treatable or preventable infections that are causing most of the deaths,” said Ramanan Laxminarayan, co-author of the study and president of the One Health Trust, a research organisation.
Overall, an estimated 7.7 million deaths globally are caused by bacterial infections, according to a previous study, representing around one in eight deaths worldwide. Preventing these infections in the first place could help with drug resistance, he said.
“Although the series is about drug resistance, what we're seeing here is that yes, that's the problem, but actually, even before you get to that, there's a lot of deaths that could be averted just with things that we already know how to do,” said Laxminarayan, who is also a senior research scholar at Princeton University in the US.
Improving infection control in healthcare facilities through hand washing and regular cleaning could save nearly 340,000 lives a year, the researchers estimated.
Access to drinking water could prevent another 247,000 deaths while access to paediatric vaccines could save 181,500 lives, they added.
The researchers will present the series next week at the World Health Assembly in Geneva, which brings together all members of the World Health Organization (WHO).
New targets to tackle anti-microbial resistance
The research series also includes suggested targets for antimicrobial resistance to be discussed during a high-level meeting amid the UN General Assembly in September.
The goal is “10, 20, 30,” including a 10 per cent reduction in mortality from antibiotic resistance by scaling up measures to prevent infection.
They also recommend a 20 per cent reduction in “inappropriate human antibiotic use,” such as using them for mild respiratory infections, and a 30 per cent reduction in inappropriate use of antibiotics in animals, such as for promoting growth.
These targets are “feasible, but they're ambitious at the same time,” Laxminarayan said, adding that better use of appropriate antibiotics for people with limited access could help.
“We're saying everyone should have access to antibiotics that are effective, but we're also saying that inappropriate use needs to come down by 20 per cent. Those are simultaneously possible, because many people are using antibiotics that are not appropriate,” he said.
Any new antibiotics need to be made accessible and affordable for patients, he added.
‘Health systems ill-prepared’
In a linked comment alongside the series, 12 people impacted by antibiotic resistance say that as there are many drug-resistant pathogens, data collection can be a challenge.
One of the co-authors of the linked comment, Nour Shamas, a member of the WHO’s task force of antimicrobial resistance survivors, said in a statement that her mother had developed an infection from drug-resistant bacteria in her kidneys and urinary tract after surgery.
“In Lebanon, as in many countries, our health system is ill-prepared to protect patients against AMR – there are gaps in effective infection control and sanitation practices, significant medication shortages, and antimicrobials, if available, are often prescribed for inappropriate uses,” she said.
“My mother is only one example of the millions of patients globally who develop an antimicrobial-resistant infection whilst in hospital each year,” she said, calling for reducing infections and antibiotic resistance to be made an urgent global priority.