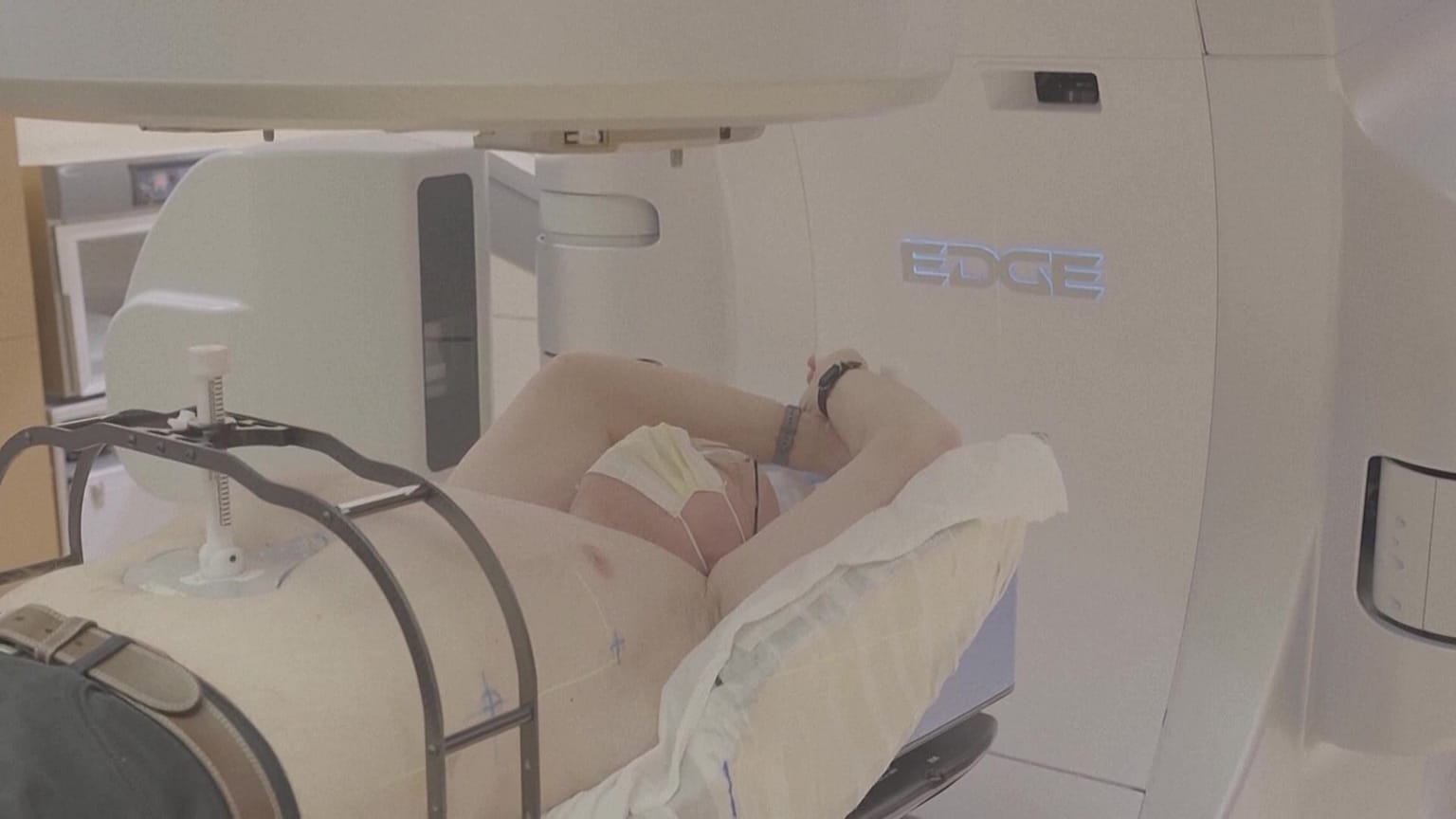
Radiation normally reserved for cancer patients is being tested on 400 patients to see if it helps repair misfiring heart cells.
A major cause of sudden cardiac arrest, ventricular tachycardia, is thought to be responsible for about 6 million deaths annually worldwide.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
The heart’s abnormally fast heart rhythm prevents it from properly pumping blood as a result of electric signals that short-circuit in the bottom chambers, the ventricles, often because of damage from a prior heart attack.
This life-threatening condition can be treated by threading catheters inside the heart, burning the misfiring tissue, and creating scars that block bad signals – a procedure called catheter ablation.
The problem with catheter ablation is that some patients are too sick for it, while others relapse.
Researchers at Washington University are now testing radiation therapy, which is normally used for cancer, in a bid to find an alternative to heart surgery.
Treating the heart with radiation is a radical approach. Cancer doctors are normally trained to avoid radiating the heart at all costs for fear of collateral damage.
But as part of an international study, sponsored by device maker Varian, nearly 400 patients will be randomly assigned to either radiation or another catheter ablation to directly compare how they fare.
‘Gentle treatment’
Patients lie in the same machine that normally blasts cancer, held in place and listening to music while customised beams hit just the right spot. It can take as little as 15 minutes.
Researchers believe the one-time dose may reprogram misfiring heart cells to control heartbeats more like younger, healthier cells do.
"It is a gentle treatment that's completely noninvasive," said Dr Phillip Cuculich, a cardiologist at Washington University in St. Louis.
The study now aims to prove whether the quick, one-time dose of radiation really works well enough - and is safe enough - for more patients like Jeff Backus, who relapsed after standard care.
Backus had already undergone an hours-long invasive procedure to keep his heart beating properly and had a defibrillator implanted as a back-up. Then this winter, twice in about a month, Backus briefly passed out and had to be saved by his defibrillator, which shocked his heart back into rhythm.
“You’re always in the back of your mind thinking, ‘Is it going to happen?’” he said.
He chose to try the experimental radiation in February - and so far is doing well.
"At least we're trying something. And hopefully, it's going to work," he said.
How does it work?
Radiation is normally used to attack cancer while avoiding nearby healthy tissue, but for ventricular tachycardia, a moderate, one-time dose of radiation is directly zapped onto the heart.
Before the radiation therapy, a patient’s heart’s electrical activity is measured using a vest covered in about 250 electrodes.
"In just one or two beats, we can map the electrical part of the heart and we can see where is the start of that arrhythmia," Cuculich explained.
Tests with donated human hearts and mouse hearts proved how the radiation prevents arrhythmias: the one-time moderate dose of radiation was essentially prompting the misfiring cells to repair themselves.
In areas that got zapped, heart muscle cells temporarily switched on certain genes that normally are dormant in adulthood.
"It may actually rejuvenate sick tissue, and that's pretty exciting," said Dr Stacey Rentschler, a developmental biologist at Washington University in St. Louis.
"It can be thought of as turning back the clock to take a diseased tissue and perk it up and make it function more like normal," Rentschler added.
Possible long-term risks
Cuculich has, together with radiation oncologist Dr Clifford Robinson, successfully conducted experiments with small numbers of desperately ill patients since 2017.
Aiming at the heart “wasn’t on my radar at all. My goal was to miss the heart,” Robinson said. After all, some lung and breast cancer survivors experience heart disease years later from tumour radiation that reached and inflamed heart tissue.
But he agreed to try, warning patients about possible long-term risks.
His very first arrhythmia patient responded, “You're concerned about something that might happen 10 or 20 years from now? I'm worried about tomorrow,” Robinson recalled.
“That was really eye-opening,” he said.
Although this method hasn’t been officially approved by the US Food and Drug Administration, the St.Louis team has since gotten permission to treat about 80 more people including Backus.
The duo has also taught the technique to dozens of other hospitals in the US and abroad that are cautiously trying it.
But the FDA requires stronger evidence for more routine use - and the more hospitals offer “off-label” radiation to these heart patients, the harder it will be to get that proof.
Washington University in St. Louis just began recruiting potential participants for the new international study, and additional sites are set to open soon.
For more on this story, watch the video in the media player above.