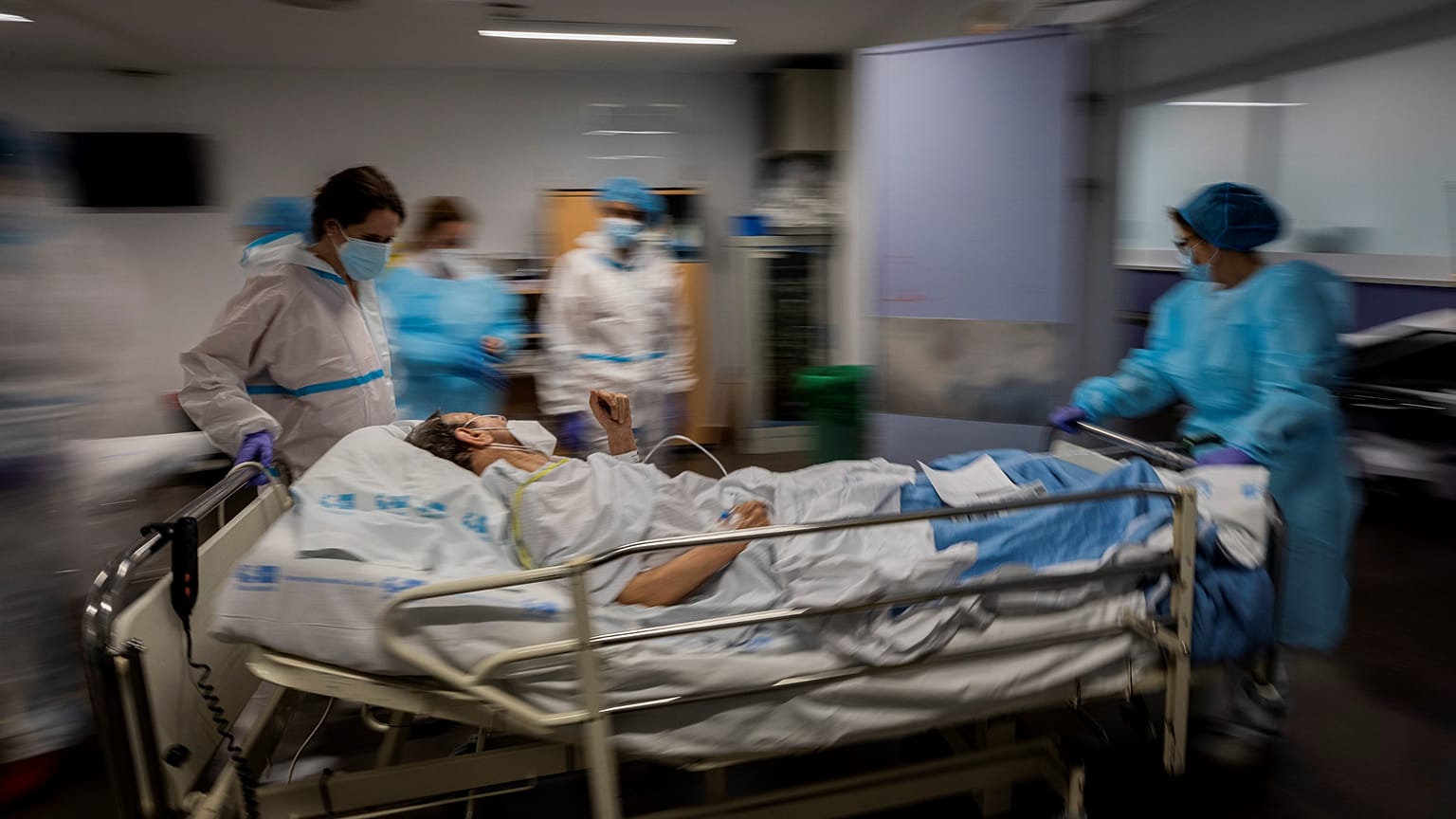
The scientists behind the tool say it could be especially valuable to resource-limited countries.
A tool has been developed to help healthcare professionals identify hospitalised patients most at risk of dying from COVID-19 using artificial intelligence (AI).
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
The algorithm could help doctors to direct critical care resources to those in most immediate need, which the developers of the AI tool say could be especially valuable to resource-limited countries.
And with no end in sight for the coronavirus pandemic, with new variants leading to fresh waves of sickness and hospitalisation, the scientists behind the tool say there is a need for generalised tools like this which can be easily rolled out.
To develop the tool, scientists used biochemical data from routine blood samples taken from nearly 30,000 patients hospitalised in over 150 hospitals in Spain, the US, Honduras, Bolivia and Argentina between March 2020 and February 2022.
Taking blood from so many patients meant the team were able to capture data from people with different immune statuses – vaccinated, unvaccinated and those with natural immunity – and from people infected with every variant of COVID-19.
With so much data, they were able to train an AI programme to predict the signs of a poor prognosis, regardless of the different immune statuses or variants.
Furthermore, they tested if the time bloods were taken affected the tool’s performance, comparing data from different time points of blood drawing before patients either recovered or died.
They found the algorithm predicted with high accuracy the survival or death of hospitalised patients up to nine days before either outcome occurred.
The resulting algorithm – called COVID-19 Disease Outcome Predictor (CODOP) – uses measurements of 12 blood molecules that are normally collected during hospital admissions, meaning the tool can be easily integrated into any hospital.
The peer-reviewed findings were published in the journal eLife.
‘More surges of hospitalisations likely’
“The appearance of new SARS-CoV-2 variants, waning immune protection and relaxation of mitigation measures means we are likely to continue seeing surges of infections and hospitalisations,” explained the leader of this international project and senior author David Gómez-Varela, former Max Planck Group Leader and current Senior Scientist at the Division of Pharmacology and Toxicology at the University of Vienna in Austria.
“There is a need for clinically valuable and generalisable triage tools to assist the allocation of hospital resources for COVID-19, particularly in places where resources are scarce. But these tools need to be able to cope with the ever-changing scenario of a global pandemic and must be easy to implement”.
Gómez-Varela added that the team were now working on a follow-up dual model “tailored to the current pandemic scenario of increasing infections and cumulative immune protection, which will predict the need for hospitalisation within 24 hours for patients within primary care, and intensive care admission within 48 hours for those already hospitalised”.
Scientists from a number of institutions were involved in the collaborative development of the tool, including the Max Planck Institute of Experimental Medicine, Turku University in Finland, the Spanish Society of Internal Medicine, The Argentinian Society of Medicine, and the International Forum of Internal Medicine.