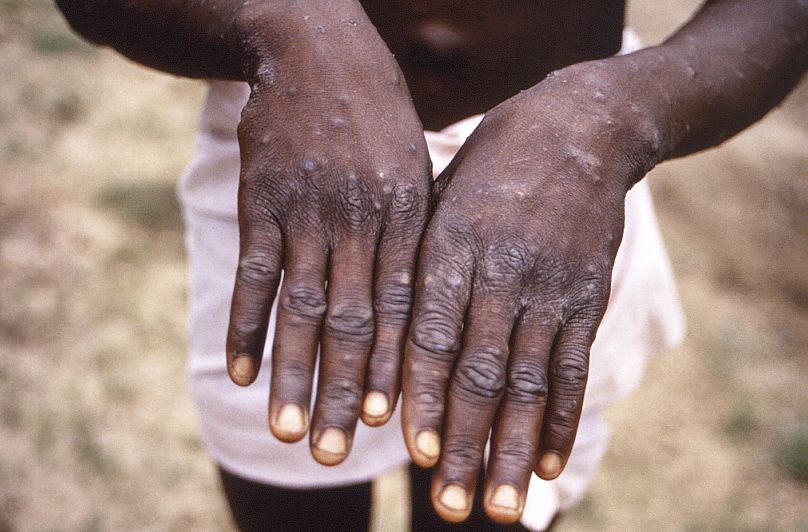
Lack of access to vaccines, stigma, and a fast-moving new variant have hindered the DRC’s mpox response.
A new strain of mpox that emerged in the Democratic Republic of the Congo (DRC) could become an international health threat if it isn’t contained soon – and while lessons from recent viral outbreaks offer a path forward, it’s unclear whether authorities will act quickly enough to rein in the virus.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
The DRC has been grappling with a major outbreak of mpox, formerly known as monkeypox, since September 2023.
But it has reached a crisis level recently because the lethal new strain is spreading without sexual contact and may be evading diagnostic tests. Cases are also reaching record highs, and vaccines are not widely accessible.
About 9,600 suspected mpox cases have been reported in eight African countries this year, and more than 400 people have died. Children under 15 have accounted for most of the new infections and deaths in 2024.
Nearly all of the cases so far have been in the DRC, but health officials say the new strain may already have spread beyond its borders, and that overall cases are likely underreported due to spotty testing and surveillance.
Without mitigation measures, mpox could soon cause more illnesses and deaths, and spill beyond Central Africa.
“There's every likelihood that the virus may be on the move,” Dr Rosamund Lewis, the World Health Organization (WHO)’s technical lead and emergency manager for mpox, told Euronews Health.
Mpox became a global crisis in 2022 when cases broke out among gay and bisexual men in Europe and North America.
This marked the first time that sustained transmission was identified outside of West or Central Africa, where the virus has been endemic for decades in some countries.
Mpox has now been detected in 116 countries. Since 2022, more than 27,000 cases have been confirmed in Europe, where the virus continues to spread among men who have sex with men.
While some people have no symptoms, mpox can cause fever, fatigue, and a rash that turns into painful skin lesions, and in extreme cases, it can lead to death. It’s particularly dangerous for children, pregnant women, and people with compromised immune systems due to an advanced HIV infection.
‘Risk for the rest of the globe’
The strain that caused the global outbreak in 2022 is called Clade II, which is typically found in West Africa and is far less deadly than Clade I, which is common in the DRC and has a case fatality rate of about 10 per cent.
The concerning new strain, an offshoot of Clade I, first emerged last year among miners and sex workers in the eastern DRC town of Kamituga.
Recently, the new strain has been found in internally displaced camps, Lewis said. It is spreading through close personal contact, not just through sex, meaning it affects a much wider group of people, making it much harder to track and contain.
Researchers say the new strain has “pandemic potential”.
“If this outbreak is not controlled, it can definitely pose a risk for the rest of the globe,” Nicaise Ndembi, a senior advisor to the director general of the Africa Centres for Disease Control and Prevention, told Euronews Health.
In 2022, health authorities got the global outbreak under control through targeted distribution of vaccines and antiviral treatments, as well as effective health messaging to at-risk communities that helped them make decisions that slowed the spread.
By February 2023, nearly 337,000 vaccine doses had been administered in the European Union, Iceland, Liechtenstein, and Norway.
But there have been barriers to this approach in the DRC and broader region, given the stigma associated with mpox and the lack of access to vaccines and treatments.
There are three mpox vaccines available globally, but the DRC just granted emergency authorisation to use two of them last week. The country has a weak system for approving medical products and the WHO doesn’t recognise the DRC’s medicines regulator as a “stringent regulatory agency”.
Dr Nelson Aghogho Evaborhene, a vaccinologist at the University of the Witwatersrand in South Africa, added that some countries lack the “technical and financial resources” needed to evaluate medicines, instead relying on WHO, other global health groups, and other countries’ regulators to determine vaccine safety and efficacy.
Domestic vaccine manufacturing is also almost nonexistent meaning the DRC, and indeed much of the region, are reliant on donated doses from other countries.
That prompted officials and researchers to warn that the public health response to mpox reflects a failure to heed lessons from the COVID-19 pandemic and the earlier mpox outbreak, when wealthier nations stockpiled vaccines for their own citizens.
“There was a huge disparity for antivirals and for vaccines,” Evaborhene said.
It’s also unclear how effective the existing vaccines are against the new mpox strain, which appears to be evading diagnostic tests. Meanwhile, clinical trials are underway to test how well the vaccines work to protect children.
Need for public health infrastructure in Africa
Ndembi said more research is needed, but that given the emergency situation, African officials should prioritise getting the existing vaccines out quickly in countries with mpox transmission.
With immunisations not yet widely available, Lewis said better disease surveillance, targeted public health messaging, and clinical care for infected patients would help get the outbreak in check.
She also said mpox testing and treatment should be incorporated into sexual health services because it can look like herpes or syphilis.
“If you’re talking about an adult who has acquired mpox through sexual transmission, then that person should have an HIV test,” Lewis said.
While HIV isn’t a risk factor for mpox, people with HIV are at higher risk of severe illness and death from mpox.
Ndembi said the current outbreak underscores the need for a strengthened, centralised public health infrastructure in Africa, as well as health workforce development, increased regional vaccine manufacturing, more domestic funding for health security, and greater collaboration with global health organisations and other countries.
The Africa CDC proposed this roadmap, called the New Public Health Order, in 2021 after the COVID-19 pandemic exposed staggering international health inequalities.
But it has been sluggish to get off the ground, and Ndembi said the continent’s medical regulatory pathways remain “fragmented”.
“We learned the hard way during COVID, and we came to realise we need to reshape the global health architecture,” Ndembi said. As those efforts slowly ramp up, “the immediate solution here is going to be ensuring that we have access to the biomedical interventions” for mpox.
“It’s extremely important at this particular juncture,” Ndembi said.