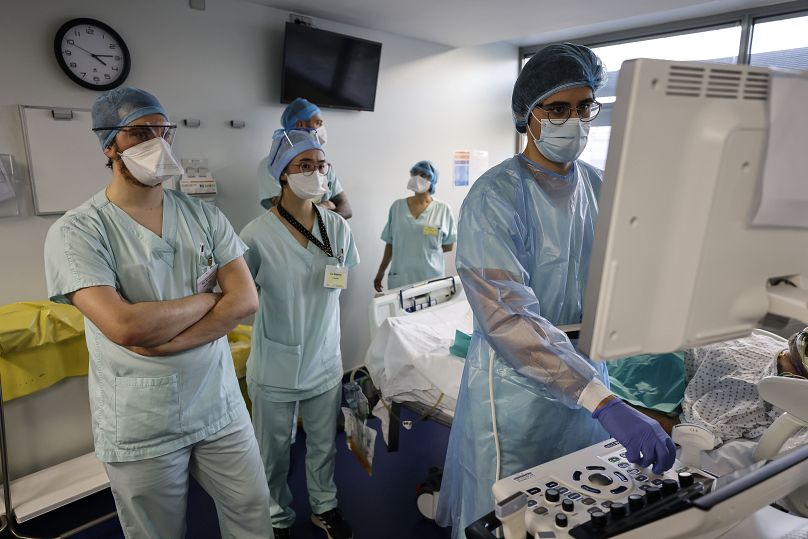
The fallout of the COVID-19 pandemic, along with ballooning health costs, are putting Europe’s healthcare systems under more strain than ever.
The COVID-19 pandemic, and ballooning health costs, are putting Europe's healthcare systems under more strain than ever.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
What should the European Union, its member states, and their citizens do to mitigate this?
Euronews brought together a panel of experts to discuss these often contentious issues, with views from elected politicians, intergovernmental and non-governmental organisations represented.
You can watch the entire debate in the video player at the top of this page.
One view that was largely agreed across the panel was that cooperation following the outbreak of the COVID-19 pandemic wasn’t successful enough across Europe. That experience has however shown the importance of a European Health Union, and maintaining good communication and cooperation on health within the bloc, the panellists said.
The panel consisted of:
Tomislav Sokol - MEP EPP Croatia
Martin Smatana - Associate fellow for health and economic growth programme, GLOBSEC
Josep Figueras - Director, European Observatory on Health Systems and Policies
Cyrus Engerer - MEP S&D Malta
Even before the added pressure from COVID-19, Europe was facing other issues. It has an ageing population, and as economic uncertainty grows across the region and budgets tighten, there is growing concern about a sector that touches all of our lives.
Lack of coordination amid pandemic
Before looking ahead to the future, the panellists took a look back at the recent difficulties the COVID-19 pandemic inflicted on health systems across Europe.
“In the beginning there was a lack of coordination, closed borders, export restrictions and so on,” said Tomislav Sokol, a Croatian MEP. “Some member states didn’t want to export medical equipment to those who needed it most, that was a big problem.”
For Cyrus Engerer, a Maltese MEP, a major issue to highlight was all the missed diagnoses caused by the pandemic interrupting day-to-day healthcare.
“Now is the time we’re seeing a section of the population that will probably never be diagnosed because they have passed away,” he said.
“If you see people who are over the age of 65, 70, who would have been diagnosed with some kind of cancer or other critical illnesses, probably and we are seeing it right now, there is a gap. Who are those people? What we’re learning today is those are people who have passed away.”
Martin Smatana, Associate fellow for health and economic growth programme, GLOBSEC, said his biggest critique of the EU’s response was that the health union “should have been more ambitious, and go into other areas that we know are going to cause problems,” which he said was first and foremost a shortage of doctors, nurses and other healthcare workers.
Workforce under pressure
The panel agreed the issue of human resources was something that must be prioritised.
“We all believe in digital, but its human resources, the training, the culture, the incentives, the regulation, it's not just pouring money into new digital tools and gadgets and infrastructures,” said Josep Figueras, the director of the European Observatory on Health Systems and Policies.
“We need to use these resources very wisely and in particular with the health workforce,” he added, pointing out that when it comes to mental health, as many as 50 per cent of the workforce in some health systems are suffering from PTSD and stress.
“So one of the silver linings is actually realising finally the need to support the health workforce. Now we do it, or we are really in trouble.”
Cyrus Engerer was in agreement about the risk facing human resourcing in healthcare. “Everything is interlinked,” he said.
“We mentioned the workforce. The EU is losing out on talent because, when it comes to getting more nurses, doctors, healthcare professionals, we have a system which is blocking these people for coming to the EU, and what are they doing instead, they’re going to the US, to the UK, they're going to Australia, Canada and Japan."
Who should pay for healthcare?
The debate over who should have to pay for healthcare was more polarised. Engerer argued healthcare should be free for every EU citizen, saying: “ “I’m always a bit afraid when we discuss healthcare insurance, paying upfront and then getting refunded…in my opinion free healthcare is essential.”
Josep Figueras responded that while “we are all singing from the same music here…the reality is very different. Who's going to pay the bill for patients from the east being treated in Germany or in the West?”
This tied into the conversation about the EU aiming for a tobacco-free generation by 2040.
In 2017, over 91 per cent of deaths and almost 87 per cent of DALYs (healthy years lost) within the EU were already the result of non-communicable diseases, according to data from the Global Burden of Disease study (WHO).
Tobacco use was identified as a top risk factor, alongside unhealthy diets, harmful levels of alcohol consumption, and physical inactivity. In the EU, tobacco consumption is the leading cause of preventable cancer, with 27 per cent of all cancers attributed to smoking.
Harm reduction
Cyrus Engerer argued that tackling tobacco smoking should start with harm reduction.
“Now, I'm not saying that alternatives to tobacco products are something good, but let's start reducing harm and we need to start pushing towards that,” he said. “It could be e-cigarettes, it could be others as a means.”
He added that the idea was not for young people to start using e-cigarettes, which would be “very dangerous”, but to get current smokers to reduce harm to themselves by transitioning to e-cigarettes which are much less harmful.
This could be done by stopping certain advertisements, and ensuring cigarettes and e-cigarettes had effective packaging.
Tomislav Sokol agreed that transferring to alternatives to cigarettes “can really help people”.
“These alternatives are less healthy than if you don't use anything at all, right. But this is the wrong comparison, because you should compare these alternatives to actually smoking a cigarette…which is much worse than this,” he said.
He called on European health chiefs to stop only comparing people who use e-cigarettes and people who don’t use any tobacco products.
“I think that we should try to change this paradigm and try to engage more about these possibilities and alternatives, because if we do not do that, the final results will be worse.”
Martin Smatana pointed to the example of New Zealand, which has banned the sale of cigarettes to anyone born after 2009.
“Roughly 20 years ago they realised that the smoking prevalence amongst adolescents was roughly 27 per cent, and they realised the need to invest heavily and they started with a prevention mechanism, education in schools, and massive campaigns," he said.
" So they've limited the place where you can buy cigarettes, then they changed the way how the packaging can work, how flavours can work. And eventually at the end they started to play, just let's call play with taxation so it's less accessible. And at the end, as of today, the prevalence of smoking amongst adolescents is roughly 5 per cent."
But Sokol rebutted: “Is there smuggling there? In Croatia if tomorrow we prohibited selling cigarettes completely, we already have this big black market in neighbouring countries, the whole market would just go underground.
He instead advocated for prevention, as the “most cost-effective investment in healthcare.”
“It has the best results with the least amount of investment,” he said. “But the problem is the results take a long time, and most politicians only look at one, two, three, four, five years ahead, that’s the major issue.”
Josep Figueras said that Europe is not doing a good job of regulating tobacco and the harms it causes, insisting he would push for “far more”, including requiring a medical prescription for vaping.
"We see a young population that never smoked and now they are vaping. So we are getting a new generation addicted to that.
He agreed with the ideal of harm reduction, but insisted: "We are not doing very well regulating it or making it accessible to only those who need it. For instance, shouldn't we have it by medical prescription?"
If they could change one thing today
Asked if they could improve one thing in healthcare today, Martin Smatana’s answer was that he would be happy if the European Health Union was more ambitious, and wants to see it prepare a joint human resources sustainability plan for the bloc.
Josep Figueras agreed that a sustainable and healthy health workforce was essential, but he also reminded the politicians on the panel that they have an opportunity to put health at the centre of the debate. “Health is good for security, health is good for cohesion, it's good for the economy,” he said.
Tomislav Sokol said: “The crucial thing here in the Brussels bubble is to maintain the momentum on health, at the centre of the debate. You cannot do anything without the political will.”
And Cyrus Engerer insisted: “Without a healthy population, a healthy environment, a healthy biodiversity, everything else is irrelevant.
“We have to put health at the centre of our discourse, we need to invest in health policy, we need to invest in working together when it comes to a European Health Union, and this is what ultimately joins everything together.”