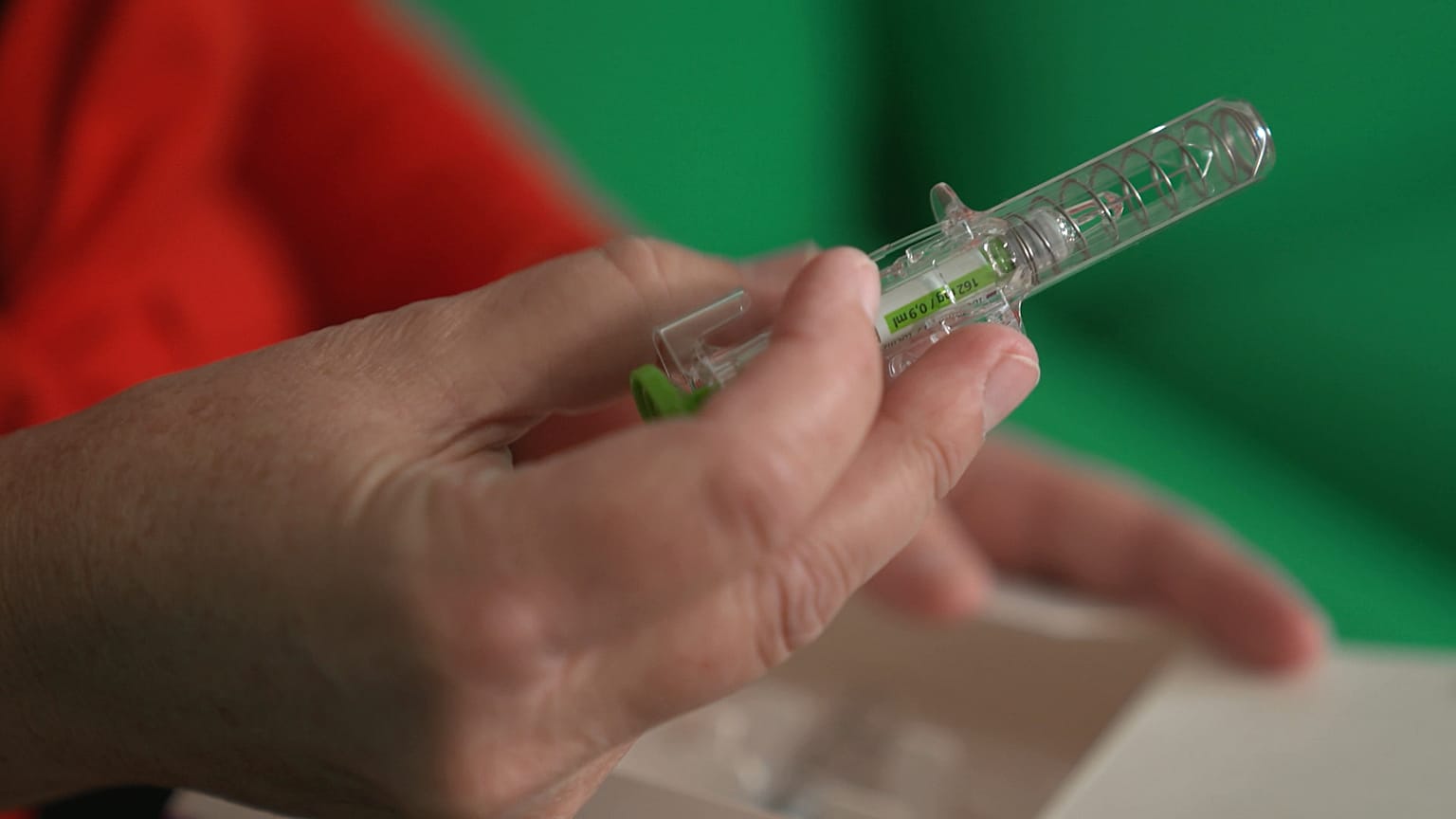
The European Commission's pharmaceutical reform would improve access to cheaper biosimilar medicines and speed up the time it takes to access the market.
Connie Ziegler was diagnosed with rheumatoid arthritis when she was a young girl.
 ADVERTISEMENT
ADVERTISEMENT
 ADVERTISEMENT
ADVERTISEMENT
"When I was about a year and a half, I was told by my parents that my knees especially started hurting. And that I didn´t want to walk very far. And started having pain. Not that long after that and the first symptoms, I was diagnosed with juvenile rheumatoid arthritis"
She began treatment for her condition in her early twenties. Then, some ten years ago, doctors advised them to change her ordinary medication to biosimilars.
Biosimilars are biological medications that are copies of approved reference drugs, though cheaper to manufacture and more affordable for patients and health systems.
We went to find out what they were.
What are biosimilars?
The European Medicine Agency defines biosimilars as " a biological medicine highly similar to another biological medicine already approved in the EU (called 'reference medicine') in terms of structure, biological activity and efficacy, safety and immunogenicity profile (the intrinsic ability of proteins and other biological medicines to cause an immune response)."
They are similar to name-band medication (reference medication) as they both contain biological material in their composition (such as bacteria, yeast or protein for example), though biosimilars will present some variations in their active substance compared to the name-brand drug. This is due to the biological nature of the medication. Biosimilars are unlike 'generic' versions of biological medicines as those are exact chemical-based copies of a name-brand drug.
However, Biosimilars are still subject to strict EU testing and approval before entering the market. They are evaluated by the EMA's scientific committees which look at the majority of marketing authorisation applications for biosimilar medicines. The medications are evaluated according to the same standards of pharmaceutical quality, safety and efficacy that apply to all biological medicines approved in the EU.
When are they used?
Biological medicines and biosimilars offer treatment options for patients with chronic and often disabling conditions such as diabetes, autoimmune disease and cancers.
"In different periods in my life, it took quite a while to find the right medication that worked for me. So I was concerned when I was told that I was going to switch to a biosimilar, would it work just as well?" explains Connie Ziegler. "I needed to address this to my physician. But I also thought, well, they would not give it to me if that was not OK. So of course I was willing to try it. There was another package, and it looked a bit different. But for me, I did not have any changes in the way I was treated or the things how I felt."
Like Connie, thousands of Danish patients have successfully switched to biosimilars these last years. Denmark has been a frontrunner in their use. The country also has a good tradition of monitoring its patients.
Biosimilars in the EU
The EMA authorised the first biosimilar back in 2006. Since then, 105 have been approved in the European Union.
Other candidates are under strict scrutiny, says EMA´s Chief Medical Officer, Steffen Thirstrup.
"What we are looking for here is to reassure (the public) that the manufacturer can produce these products in a consistent and safe manner. That they deliver what they promised to produce and that they have demonstrated that the product, from a molecular basis, is similar to the reference product. Some critics and some who would have doubts about biosimilars would argue that the standards are lower. But that is absolutely not right. We would put the same standards independently on what type of medicine we are dealing with. When generics were introduced 30 or 40 years ago, we had the same concerns. There are still rumours from time to time that generics because they are cheaper, offer lower quality. And that is not true".
Impact of Biosimilars
So as soon as biosimilars were available, experts started studying their impact. Senior consultant for Rheumatology, Bente Glintborg was involved in a number of those studies.
"When the biosimilars came on the market, it was quite obvious for us to then look at this data in a prospective manner: Say, OK, these patients they switched from one drug to another. So how do the patients´ outcomes behave, how is the drug effectiveness, is it the same?" she explains.
She and her team investigated the results of over 1,000 patients who switched to biosimilar medication compared to a baseline group treated with the reference medication the year before.
"The outcomes were very much identical. We could hardly disentangle the lines. So that illustrated to us that the patients' systems accepted this switch to the biosimilar drugs and that they had the same outcomes as they would have had on the original drug," she adds.
Acknowledging these breakthroughs, the European Commission´s pharmaceutical reform wants to improve the availability of biosimilars and generic medications to ensure that more patients can access even more affordable medicines.
According to the European Commission, modulated incentives should allow biosimilars to enter markets up to 2 years earlier than today.
From the Netherlands, the European Medicines Agency will keep playing key roles at consultation and regulatory levels.